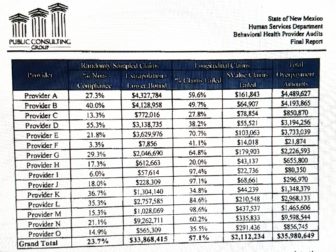
The far right column shows how much each of the 15 providers was accused of overbilling Medicaid in the 2013 PCG audit, for a grand total of $35,980,649. (Provider A) Presbyterian Medical Services $4,489,627 (Provider B) Valencia Counseling Services Inc. $4,193,865 (Provider C) Easter Seals El Mirador $850,870 (Provider D) Pathways Inc. $3,194,256 (Provider E) Hogares, Inc. $3,733,039 (Provider F) Service Organization for Youth Inc. $21,874 (Provider G) Border Area Mental Health $2,226,593 (Provider H) Counseling Center of Alamogordo $655,800 (Provider I) Partners in Wellness LLC $80,350 (Provider J) Youth Development Inc. $296,970 (Provider K) Southern New Mexico Human Development $1,348,379 (Provider L) Counseling Associates, Inc. $2,968,133 (Provider M) Southwest Counseling Center Inc. $1,465,606 (Provider N) Teambuilders Counseling Services, Inc. $9,598,544 (Provider O) Families and Youth, Inc. $856,745
Two more behavioral health providers are contesting in state court how much, if anything, they owe the state of New Mexico for allegedly overbilling Medicaid, the Santa Fe New Mexican reported this weekend.
The appeals are the latest in the drawn-out unraveling of the case Gov. Susana Martinez’s administration made in public four years ago when it charged 15 behavioral health organizations with potentially defrauding the state’s Medicaid program.
The New Mexico Attorney General cleared all 15 organizations of fraud. As New Mexico In Depth reported earlier this summer, the battle now is over how much each organization owes the public health insurance program for low-income residents.
Since 2013, when the state Human Services Department alleged the 15 providers had potentially overbilled Medicaid by as much as $36 million, HSD’s estimate of what the 15 organizations overbilled has shrunk to a fraction of that original number.
That is certainly true of Border Area Mental Health and Counseling Associates, the two providers that recently appealed the decisions by administrative law judges to state court. The rulings by the judges, who are employees of the Human Services Department, said the two owed a fraction of the $2,226,593 and $2,968,133 Border Area Mental Health and Counseling Associates, respectively, were accused of overbilling originally.
In addition to the state’s dramatically smaller overbilling estimates, HSD’s sudden change of course with two of the 15 accused providers in the past year has left the providers and longtime observers scratching their heads.
In May the state reduced to $484.71 what it said Southwest Counseling Center owed after accusing it of overbilling Medicaid by as much as $2.8 million as recently as January.
And in the fall of 2016, the state agency closed the books on another organization — Las Cruces-based Families and Youth Inc. — without demanding any reimbursements for overbilling and releasing $1.4 million in Medicaid dollars the state had suspended.
The sudden reversal appears to have occurred because the state agency found a 2012 agreement between FYI and the office of the Attorney General’s office.
The agreement was signed in late 2012 following the state Attorney General’s Medicaid Fraud Control Unit’s investigation of FYI after the organization discovered and self-reported billing problems. The Attorney General’s investigation of FYI records covered most of the period the state would later ask Massachusetts-based PCG Inc. to examine.
The agreement released FYI from any liability, civil or criminal, for the period of November 2009 through May 2012, or roughly three-quarters of the period examined by PCG.
The state would later use PCG’s findings to make ‘credible allegations of fraud’ against the 15 providers and to come up with the original overbilling estimates.