
New Mexico’s COVID-19 cases increased to 191 today, 17 people are hospitalized, one person has died. And now, the governor wants the U.S. Department of Defense to set up a staffed 248-bed combat hospital in Albuquerque.
Lujan Grisham wrote it’s “urgently needed” in a letter to Defense Secretary Mark Esper because COVID-19 might overwhelm New Mexico’s medical facilities.
That’s where New Mexico stands at the moment, and the combination of those stats, not to mention all the data and modeling that’s swirling around the internet, might make you anxious.
Many turn to data to help them understand the world. But the big problem with data about COVID-19 is the gaps. There are many. Still, as insufficient as available data is, what we do have may provide much-needed perspective.
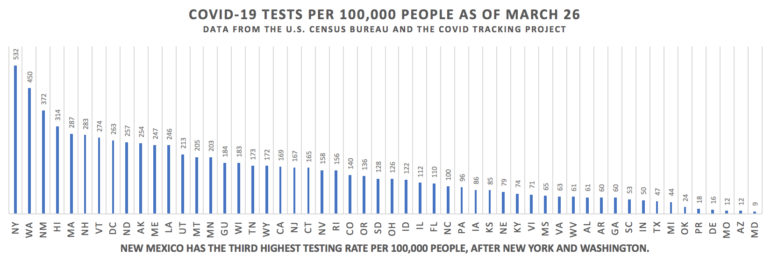
New Mexico In Depth compared U.S. Census bureau state population numbers to data compiled by the Covid Tracking Project. There’s some data missing, due to gaps in what individual states are reporting. But there’s enough to show New Mexico in the top tier of states for tests conducted per 100,000 people, according to our analysis and that of others. Even though the state hasn’t near enough testing capacity, leaving most who want one high and dry, it seems to be doing as many as it can. The more testing we’re able to do the better, because that helps officials trace and hopefully contain the virus.
New Mexico also has one of the lowest positive test rates. In other words, the percent of tests in New Mexico coming back positive is very low compared to other states. New Mexico’s positive test rate is 2% today, very low comparatively. It was one percent just yesterday morning.
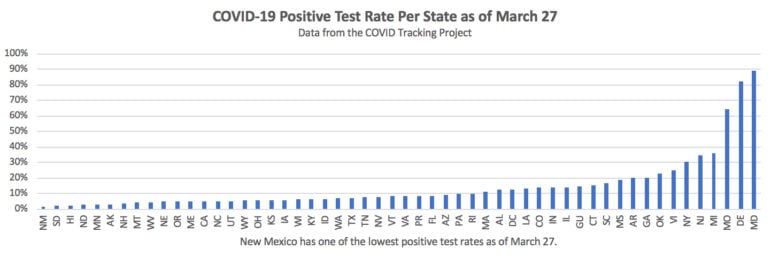
In an interview Thursday, Dr. Chad Smelser, deputy state epidemiologist, agreed New Mexico’s positive test rate is low.
One possibility for that, he said, is the state tests a greater range of people.
“In the state of New Mexico, we’ve taken the approach of testing more people than other surrounding states,” he said. “If you focus your testing only on the very sickest patients who have no other explanation for their illness, you’d expect to have more of those test positive in that population. When you expand to a greater number of people, people with milder symptoms, on occasion we had people tested who had no symptoms, you would expect the rate at which your test is positive to be lower.”
Another possible explanation for the low rate, he said, is that there’s not an “overwhelming” amount of the virus in New Mexico, right now, although officials are seeing it throughout the different regions of the state.
Smelser noted that there are models circulating on the internet with projections about how many people may eventually get the disease, and how many could be expected to die. He said he and his colleagues evaluate those models for applicability to New Mexico but cautioned that they can’t be applied in cookie cutter fashion. The state is geographically large with a small population. Mashing it up in the same models as hyper-dense New York City doesn’t help New Mexicans understand how COVID-19 will spread in their state. The DOH and its partners are working to come up with New Mexico modeling, he said, that takes into account density, demographics, and other factors specific to the state.
In the end, available data and models at our fingertips about COVID-19 are insufficient. We simply lack the data we need, which is unnerving for people who turn to data–many of us –to make sense of the world.
But there is one data point Smelser sounded very definitive about.
“The safest message is that a single case can lead to further spread,” he said.
With more testing there will be more positive test results. Looking at cumulative numbers reported by the New Mexico Department of Health shows how the number of tests and positive results have swerved skyward since March 4.
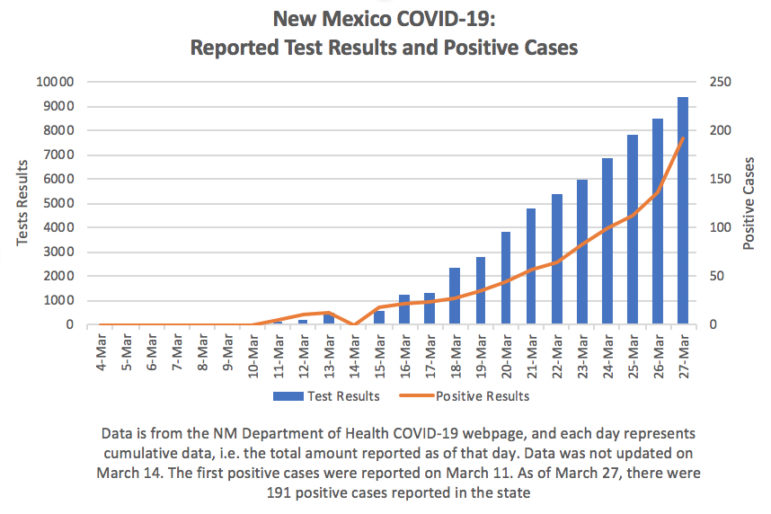
It’s that curve upward that authorities are so diligently trying to flatten through social distancing and isolation policies for the general public. It’s the data we are urged to take to heart.
Studies have shown that New Mexico has fewer hospital beds than the national average. Given that, even if New Mexico’s infection and hospitalization rates ultimately are low compared to other states, its hospitals may still not have enough capacity for very ill patients who will need ICU beds and ventilators for survival if there’s a need all at once.
That’s a likely reason Lujan Grisham began very early ordering businesses closed and urging New Mexicans to stay at home, so as to slow the rate of infection. And why now, she’s called for an Army hospital in New Mexico.