Hospital employees across New Mexico are testing positive for the virus that causes COVID-19. A survey of several hospitals this week by NMID found just under 20. But that’s likely an undercount as state officials and many hospitals are refusing to disclose how many healthcare workers have the coronavirus.
A spokeswoman for Presbyterian Healthcare Services confirmed Thursday 13 employees have tested positive across its statewide network — up from just two reported cases last week. Other hospitals confirmed a handful of infected employees. But two large health care systems— UNM Hospital and Lovelace — are keeping mum about their own numbers.
Hospital employees at Presbyterian and elsewhere are worrying about becoming sick themselves or spreading the virus to others as their employers ration masks and other personal protective equipment for an anticipated surge in cases across the state.
At UNM Hospital in Albuquerque, workers publicly protested outside the hospital Wednesday over lack of equipment, hazard pay, and administrative leave for workers quarantined due to COVID-19 exposure or illness.
New Mexico In Depth spoke to several Presbyterian employees, unnamed in this article so they could speak frankly about the shortage of protective equipment hospital workers face.
The Presbyterian hospital system, which was caring for 32 hospitalized COVID-19 patients statewide as of Thursday, anticipates a COVID-19 patient surge beginning April 20, although that could be revised, said Jeff Salvon-Harman, M.D., Presbyterian’s chief of patient safety and medical director of infection control.
According to an April 9 Presbyterian memo obtained by New Mexico In Depth, statewide hospital bed shortages are expected by late April. Hospitals are prepared to coordinate the transfer of patients between facilities as needed, Salvon-Harman confirmed. Presbyterian has begun to share publicly available information with its workers to help “psychologically prepare” them for the possibility of ventilator and hospital bed shortages, he said.
Like other hospital systems across the state, Presbyterian is struggling to deal with worldwide supply shortages.
The April 9 Presbyterian memo notes that “12 supply chain specialists are working around the clock to secure PPE” and that a “large supply of reusable P100 rubber masks with cartridges are being stockpiled for [the] surge.” PPE is common shorthand for personal protective equipment.
“Our supply chain folks have just been absolutely amazing, working 24/7, tracking down every available opportunity to acquire approved and certified medical-grade PPE for our staff,” Salvon-Harman said.
But asked if the reusable rubber P100 elastomeric respirator masks and cartridges have yet been shipped or delivered to Presbyterian, Salvon-Harman would only say that “they are in the supply chain.”
“I can’t go into detail on that because we’re still working through our communications and distribution management processes within Pres,” Salvon-Harman said, adding the masks should be delivered before the anticipated April 20 surge.
Presbyterian memos indicate that face masks, face shields, and N95 respirators are being collected as an emergency backup supply for the anticipated patient surge, in case hospitals run out of new supplies. The hospital is decontaminating them with UV light and vaporized hydrogen peroxide to destroy viruses. Nurses’ and doctors’ use of facial cosmetics such as foundation, blush or lipstick, as well as sunscreen, are now discouraged at Presbyterian facilities because they can damage masks and preclude reprocessing.
Some Presbyterian employees are concerned.
“I am alarmed at the lack of PPE,” said one Presbyterian Hospital employee, who asked not to be identified. “It’s obvious from the conservation efforts that when we get to the surge, we’re probably not going to have the PPE we need to keep ourselves safe.”
Currently, as is also the case at other hospitals across the state and nation, Presbyterian workers are required to ration their personal protective equipment, including in some cases wearing the same gear as they shuffle between patients with and without COVID-19, employees said.
Asked about that concern, Salvon-Harman said workers caring for suspected or confirmed COVID-19 patients “would change out of their PPE” before subsequently providing care to a patient who does not have COVID-19.
But that is not always happening, one nurse told New Mexico In Depth. Unless nurses are issued a new mask for each patient known or suspected to have COVID-19, or unless nurses are assigned to care exclusively for only one patient during a shift, N95s “are being used between patients,” that nurse explained. “In my department, we are still using one mask between multiple patients.”
In the ER, for example, all patients with respiratory symptoms — some of whom might have COVID-19 and others who don’t — are treated in the same area by workers who don’t change their masks, one nurse noted.
Sick workers
The “13 employees statewide who have tested positive for COVID-19, with six recovered,” and the people who came into contact with them have been told to self-quarantine until they are symptom-free and can return to work, Presbyterian spokeswoman Amanda Schoenberg wrote in an email. Officials were not able to immediately confirm if workers who have tested positive for COVID-19 are retested after their 14-day quarantine, before returning to work.
The Presbyterian hospital network is one of the largest in the state.
Presbyterian officials would not specify how many of their employees’ cases were hospital work-related infections or how many required hospitalization or the use of ventilators, citing employee privacy concerns.
Nationwide, at least 9,282 U.S. COVID-19 cases had been diagnosed among health care workers as of April 9, according to an analysis published Tuesday by the U.S. Centers for Disease Control and Prevention.
A Presbyterian nurse has been intubated for ventilator support, claimed one of the Presbyterian employees with whom New Mexico In Depth spoke.
UNM Hospital and the Lovelace Health System, other large medical systems, have declined to disclose how many of their health care workers have contracted the virus.
State officials have been similarly secretive about the number of health care workers with COVID-19 in New Mexico. In March, the New Mexico Department of Health initially denied that any health care workers had tested positive until New Mexico In Depth provided information about a COVID-19 positive physician at the Raymond G. Murphy VA Medical Center in Albuquerque.
The New Mexico VA Health Care System has had three employees test positive for COVID-19, of whom two have recovered, spokeswoman Jessica Jacobsen reported in an email Wednesday. A spokesman at MountainView Regional Medical Center in Las Cruces said one employee had tested positive for COVID-19 following travel and had self-quarantined while recovering at home. (MountainView is currently caring for two patients with COVID-19.) No workers at Memorial Medical Center in Las Cruces, or CHRISTUS St. Vincent in Santa Fe have tested positive for COVID-19, officials said Tuesday.
Rationing masks, protective equipment
Facing shortages, hospitals across New Mexico, including Presbyterian, are devising strategies for conserving limited stocks of masks.
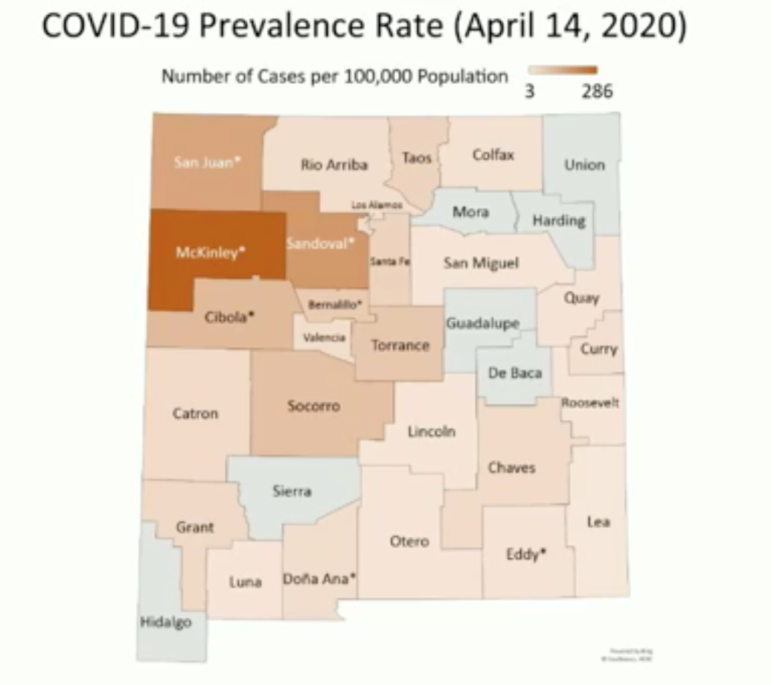
The San Juan Regional Medical Center in Farmington, where an official declined to say if any employees had COVID-19, has announced publicly it is accepting donated masks and surgical caps because shortages are so dire. Northwest New Mexico is projected to be the first region of the state hit by the anticipated patient surge, according to state officials.

Presbyterian Hospital in downtown Albuquerque has resolved shortages of eye protection but face masks and N95 respirators continue to be rationed, employees said.
An April 3 memo to staff at all Presbyterian facilities allows employees to wear “procedural” face masks throughout the day and for clinical staff to replace or upgrade to more protective N95 respirators “as patient care needs and isolation status require.”
Salvon-Harman confirmed Thursday that remains the hospital’s policy. (He explained that unlike “surgical” masks, which have string ties, procedural masks have elastic bands and are more readily obtained.) Visitors who arrive at the hospital without masks are now also provided a procedural mask, he said.
However, N95s are frequently “brown-bagged” in paper lunch sacks between encounters with COVID-19 patients, Salvon-Harman and employees said — a CDC-recommended COVID-era shortages-related rationing strategy widely used at hospitals across the nation. (The decision of whether or not to bag masks between patient encounters is left to clinicians’ discretion, Salvon-Harman said.)
One employee questioned the safety of the practice. The idea is to orient the N95 such that the contaminated outer surface of the respirator always touches the same interior surface of the bag. But “the bag interior is contaminated and in practice, nurses reuse the same bags to store their N95s between use with multiple patients,” that employee noted.
Salvon-Harman said paper bags do not retain moisture to the same degree as plastic bags but acknowledged that he knew of no research specifically showing that paper bagging is safe and effective.
N95 respirators are designed for one-time use only. However, Salvon-Harman noted recent research showing that N95s can be safely decontaminated for reuse and that their elastic bands do not become less effective with decontamination.
Workers also worried about wearing the same protective gear while caring for different patients.
Unlike the main COVID-19 intensive care unit at the Albuquerque Presbyterian Hospital, health care workers in other units must care for a mix of patients during each shift – both those with suspected or confirmed COVID-19 and patients who do not have the disease.
Moving from COVID-19 patients to other patients while wearing the same masks and other gear could put patients at risk of cross-contamination and infection, two employees said.
Salvon-Harmon, however, said that workers would change between such patients. If workers are treating COVID confirmed or suspected patients, he said, “and then went to provide care to a non PUI [person under investigation], non Covid, confirmed patient, they would change out their PPE.”
It’s unclear how workers–who have been charged with conserving their equipment–would know to change between patients who arrive at the hospital without a diagnosis, however.
When people first come to the Presbyterian Hospital ER in Albuquerque, workers can’t immediately determine whether arriving patients’ respiratory symptoms are caused by COVID-19 or other diseases, like asthma, chronic obstructive pulmonary disorder (COPD) or congestive heart failure, which can cause breathing problems. But all patients with respiratory symptoms are assessed in the same area.
“It’s difficult to know before a patient arrives if they are highly suspected of having COVID-19,” a Presbyterian Hospital employee explained. “We need to see their lab work, their chest x-rays and other diagnostics. Unfortunately, this means individuals with non-COVID-related asthma exacerbations, COPD, and congestive heart failure have been cared for by the same staff as those with known COVID-19.”
People with moderate to severe asthma have a higher risk of becoming “very sick” from COVID-19, according to a U.S. Centers for Disease Control and Prevention website. People with asthma, diabetes or heart disease are more likely to become severely ill or to die of COVID-19, according to the World Health Organization.