Printed in white block letters, the question stretched across billboards around Albuquerque last summer. And it still haunts the mother of two, Elaine Maestas, who helped pay to put them up.
“What if emergency responders came armed with compassion instead of guns?”
In 2019 when her little sister Elisha Lucero’s mental health was deteriorating, 911 seemed like the only place to turn for help. “Leash” was in counseling to manage her worsening migraines and hallucinations, Maestas said, but she was deeply afraid of being hospitalized or medicated. So as her behavior became more erratic, she resisted her family’s entreaties to seek further treatment, and they felt they had no recourse but to call law enforcement to the South Valley address where she lived.

Fishing was one of Elisha Lucero’s favorite pastimes. In April of 2016 she met up with one of her best high school friends to fish at Tingley Beach, where she caught around seven fish off corn and fireballs. Image provided by Lucero’s family.
The first time they did, the dispatcher sent a Mobile Crisis Team, which pairs an officer or deputy with a trained clinician, and the team convinced Lucero to go to the hospital. But late on the night of July 21, 2019, when her family called again, no such teams were working. And the deputies who were sent in their stead made a chaotic situation worse.
They banged on the door of Lucero’s RV, flashed lights through the windows, and ordered Lucero to “act like an adult” and come outside. After 20 minutes they were preparing to leave when she burst through the door — and they unloaded their guns into her. Lucero, who was 4’11” with her shoes on, was hit 21 times and died in the street outside her home.
Lucero is just one of a long list of New Mexicans with mental illness who needed help from emergency responders but got hurt or killed instead. Her death illustrates both the state’s unmet needs for mental healthcare, and the tragic misuse of lethal force. And it helps explain why the rate at which people in New Mexico are shot and killed by law enforcement is far higher than anywhere else in the country, fully three times the national average.
Maestas acknowledged that challenges of this complexity can’t likely be resolved at a stroke, but she believes the general direction to take is clear: “We would like to see police officers aren’t the ones responding to these calls anymore.” Their skillset just isn’t right for people experiencing these types of problems, she said. “You can’t have a foot doctor doing a brain surgery.”
***
Last summer, after the death of George Floyd under the knee of a Minneapolis police officer touched off nationwide calls to “defund the police,” Albuquerque was among the first cities to alter its approach.
Mayor Tim Keller proposed diverting some 911 calls to a new branch of emergency responders better suited for handling crises related to behavioral health, addiction, and homelessness. The agency, which he dubbed the Community Safety Department, would be staffed by unarmed clinicians rather than law enforcement, and would take “a public health approach to public safety.”
The city’s plan generated national headlines, in part because there are few cities with any kind of unarmed emergency response, let alone one institutionalized as a cabinet-level department with government employees. The most well-known, Crisis Assistance Helping Out On the Streets or CAHOOTS, operates in Eugene and Springfield, Oregon and is staffed by a non-governmental health clinic. Olympia, Washington also has a small program, and in the last year a raft of larger cities have announced their own efforts, including Denver, New York City, Philadelphia, Los Angeles, San Francisco, and St. Louis.
In an interview with New Mexico In Depth, Keller underscored the scale of his ambitions: “We are trying to fundamentally change how we respond to 911.” According to Albuquerque’s Chief Administrative Officer Sarita Nair, one of the primary goals is to reduce the risk of harm that police can introduce to situations where they are not needed.
“The strain of the ‘defund’ movement that really resonated was this concept of decriminalizing the interactions between the city and the people,” she said, drawing a comparison to a clean-up program for improperly disposed needles and syringes that the city began in 2018: agencies other than the police implemented the program in order to prevent encounters with people who use drugs from spinning into matters of criminal enforcement.
The Community Safety Department should be judged by its success resolving the underlying social problems that precipitated an emergency call in the first place, Nair said. “Instead of this model of re-responding to the same person over and over again, can we move the needle so that they are now in a better place in their lives and not generating 911 calls?”
But in the months since Keller’s first announcement, and despite a lengthy community listening process, major questions about the department remain unanswered. In mid-October when city councilors finalized a budget, they pared back the mayor’s proposed new agency to just a handful of new positions.
This effectively sent the administration back to the drawing board, to better articulate how the new department will distinguish calls to which unarmed clinicians can safely respond, and commit the resources and staff necessary to deliver services to people in crisis that truly match their needs.
***
Across the country, police officers encounter mental illness, homelessness, and addiction on a daily basis. People struggling with these challenges have few places to turn for help, and when they fall into crisis—slipping through a weak social safety net and fragmented behavioral health care system—it is often law enforcement that ends up picking up the pieces.

Elisha Lucero’s sister, Elaine Maestas, says police officers shouldn’t be first responders to emergency calls for help regarding people suffering a mental health crisis. Image by Ted Alcorn.
But in so many ways, research has shown police are unsuitable for the responsibility. They are perceived by many as threatening, and with minimal training in assessing and addressing complex behavioral health issues, they can be prone to escalating tense situations. In the most disastrous cases, police react to someone acting unpredictably by shooting them. More than a quarter of the people killed by the police each year are in the throes of a mental health crisis, according to a database of law enforcement shootings maintained by the Washington Post.
With an increasing recognition of these limitations, even police officers have warmed to the idea of unarmed emergency responders. “I’ve been on a ton of calls where I shouldn’t have been there,” said Matt Dietzel, a lieutenant in the unit that oversees many of the Albuquerque Police Department’s behavioral health activities. “We’re trained to go after criminals and people who are trying to hurt us as a result of wanting to escape, but then you have these mental health calls where it’s hard to turn off that self-preservation-fear.”
Law enforcement in New Mexico face a thornier set of challenges than most. Last year the state had the highest rate of chronic homelessness in the country, according to federal data, and has long experienced a high prevalence of addiction. Although serious mental illness is no more common in New Mexico than elsewhere, the state has lacked clinical resources ever since former Gov. Susana Martinez dismantled the behavioral health system. (In 2019 the state had to pay out $10 million to settle lawsuits from the affected healthcare providers, in addition to settling unpaid claims).
The Albuquerque Police Department (APD) is the largest of the state’s more than 100 independent law enforcement agencies and has long struggled with particular challenges of its own. Since 2014, it has been under a federal monitorship for engaging in a pattern or practice of excessive force, particularly against people with mental illness or in crisis—and the monitor’s latest report indicated that senior officers continue to resist reforms.
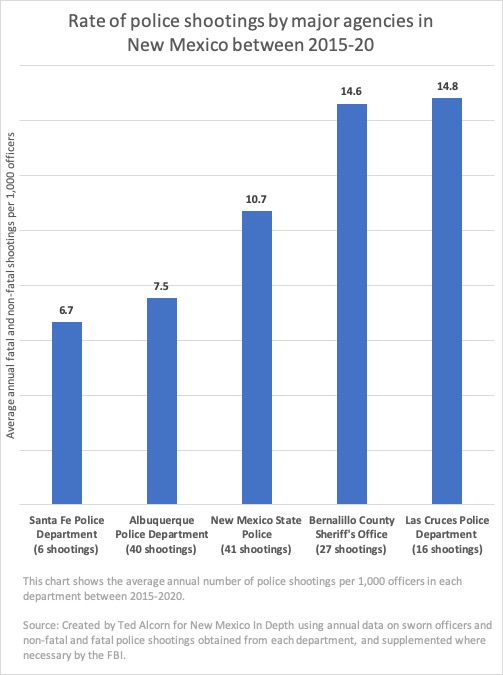
Data on fatal and non-fatal police shootings obtained from major New Mexico law enforcement agencies show that such incidents aren’t limited to Albuquerque. Between 2015-20, New Mexico State Police shot more people than APD, despite having a force that is two-thirds the size. Controlling for the number of officers, the Las Cruces Police Department and Bernalillo County Sheriff’s Office shot people twice as frequently as APD.
Albuquerque’s efforts to better address people in behavioral health crises could offer lessons for other law enforcement agencies in the state seeking to reduce police use of force — but they are far from the city’s first effort. Over the last 25 years, Albuquerque has initiated an array of initiatives bearing bewilderingly bland acronyms to better prepare officers for these types of calls or to supplement them with other types of personnel.
In the 1990s, APD began offering officers Crisis Intervention Training (CIT) — and when the federal consent decree mandated it for everyone, the department rolled out an “Enhanced” curriculum for those who wanted further training. In 2005 the department established Crisis Outreach and Support Teams (COAST), a small staff of unarmed case managers who focus on a subset of mentally ill people who come into repeated contact with police and try to connect them with social services that will prevent future brushes with law enforcement. Since 2017, 911 calls about people on the ground or unconscious (so-called “down-and-outs”) have been diverted to the fire department or transit security officers in lieu of police. And beginning in March 2018, both Albuquerque and Bernalillo County rolled out Mobile Crisis Teams (MCT) that pair law enforcement officers with licensed clinical social workers employed by the non-profit HopeWorks.
For all the good done by this patchwork of efforts, it did not add up to systematic change nor substantially improve outcomes.
When APD receives 911 calls with an explicit nexus to behavioral health, it attempts to dispatch officers who have undergone the enhanced CIT training — but they aren’t always available in the geographic areas where they are needed. Over its fifteen years, COAST has never counted more than a few staff. And the Mobile Crisis Teams are still premised on law enforcement being present — and no amount of training can absolutely ensure an armed officer who is responding to a behavioral health call won’t end up using more force than is necessary. In total, APD data show that its officers shot 40 people over the last six years, killing 24 of them.
All of which explains the appeal of a new, unarmed branch of emergency response.
***
In seeking to consolidate many existing city services into the Community Safety Department as a way to kickstart the new agency, the Keller administration’s early efforts ran into headwinds. The $7.5 million and staff of 83 requested in the administration’s first proposed budget were almost all from other parts of the city government: the police department’s COAST case managers, transit security officers, homeless outreach workers, a staff member of the city’s syringe cleanup program. As pointed out by the Albuquerque Journal, it seemed hypocritical that a department dedicated to working with mentally ill people would be devoid of mental health professionals.
Pat Davis, a city council member who was once himself a police officer in Washington, DC, said, “If you have the same number of people doing the same number of jobs with just a different logo on their shirt, we’re not really doing change.” He and other city councilors rejected most of the proposed transfers of staff and released only a fraction of the proposed funding until the mayor offered a clearer plan. Undeterred, the mayor’s office continues to develop a more ample proposal to propose to the City Council this year. This week, Keller announced that the infrastructure bond package that will be sent to voters later this fall will include $7 million for a new building for the agency.
When policymakers reconvene this spring to develop a budget for the next fiscal year, it will become clear what level of investment the city is willing to make.
Danny Whatley, a former police officer who co-chairs the Albuquerque’s Mental Health Response Advisory Committee, said that the $7.5 million the mayor originally proposed wasn’t nearly enough. “That won’t even get it started, I don’t believe.”
David Ley, the director of the non-profit New Mexico Solutions, agreed, drawing a comparison to the $184 million budget of the police department. “It’s going to be very, very difficult for a tail that small to wag the dog.”
Whatever emerges will also have to navigate the sometimes conflicting sentiments of the broader public.
Some activists hold the view that the only meaningful way to fix policing is to reduce the number of officers—which Mayor Keller adamantly opposes. When he ran for office he committed to recruiting 100 new police officers each year for a department that he said is “coming from a place of deep shortage” — even as he frames policing as just one component of a broader public safety strategy that also addresses homelessness, youth opportunity, and safe public spaces.
Melanie Yazzie, a UNM assistant professor and co-founder of the Native rights coalition The Red Nation, which advocates for reducing and eventually eliminating police and prisons, tentatively approved of the new department, but only as a stop-gap measure. “Any kind of reform that in the interim reduces harm is something we should support. But really what we are demanding is a widespread, sweeping change in our entire philosophy of how we engage with each other as a society.”
With Albuquerque’s homicides at record highs, it may be an unfavorable moment to promote a diminished police presence. “That makes it hard to talk about a vision of the future that looks different right now,” conceded Rachel Biggs, policy director for Healthcare for the Homeless. “It’s hard for people to envision what the future could look like without an armed response.”
Challenging questions face new agency

Elaine Maestas visits a memorial to her sister on the site where she was killed by Bernalillo County sheriff’s deputies. Image by Ted Alcorn.
For the new agency to live up to its purpose, it will have to clear several hurdles.
One is to determine which calls for service will be eligible for a non-law enforcement responder, which will ultimately define the department’s size and the degree to which it reduces contact between community and police.
The more cautious the city is in sending unarmed responders, the more limited the reduction in overall police-community contacts. The people who will make the distinction are the call takers and dispatchers at the city’s Emergency Communications Center, which operates out of an undisclosed location on the southwest of town. The center receives over 1.1 million calls per year, of which 375,000 are for emergencies.
Erika Wilson, who manages the center and its 140 personnel, said many calls do not ultimately merit armed law enforcement but it can be difficult to determine that in advance of arriving at the scene. CAHOOTS, in Eugene, claims it responds to 17 percent of the total calls received by its affiliated police departments—but experts say that’s a higher proportion than most law enforcement agencies attribute to behavioral health. “The reality is it’s going to be ‘some’ — and I don’t know what that ‘some’ is,” said Wilson.
Albuquerque’s 911 call data provide little clarity because they don’t capture characteristics of the incidents in their totality. (The city isn’t alone in this: a recent report by the Vera Institute of Justice showed most 911 systems fail to document the content of their calls in a standardized way.)
Wilson said a large share of calls have a behavioral health component but it’s uncommon for callers to state up-front that they are in a behavioral health crisis. That’s part of why the center categorizes just a tiny fraction of its calls as related to mental illness — around 6,000 a year. For example, a caller might report their vehicle had been stolen before adding that it was likely taken by aliens. In this case, Wilson said, the dispatcher would likely code the call as a stolen vehicle, even if they simultaneously deployed behavioral health resources.
Other categories of calls sound ripe for an unarmed response but sending one without law enforcement could be risky.
Among the 16,000 annual calls categorized as “wellness checks” are some that likely don’t require law enforcement — an absentee neighbor whose mail is piling up, or children down the street who don’t appear to be getting enough to eat — but police responding to wellness checks also encounter people with weapons. “It’s so contextual,” said Lt. Dietzel, and that uncertainty is part of why risk-averse cities continue to rely on law enforcement. “It’s just easier to say ‘send the police.’”
Mariela Ruiz Angel, the social worker who has been fleshing out the policies of the new department, said at the outset its staff will respond to only the lowest acuity calls— including abandoned vehicles, improperly disposed needles, and callers who are feeling suicidal but haven’t yet formulated a plan of action. She acknowledged that “the community would love us to go out to” more serious calls, but if there was a safety concern or a chance someone would need to be transported or taken into custody, they’d need a police officer to be there.
Assigning unarmed responders to a broader swath of calls will also require clinicians willing to fill that role — and statewide, they’re already in short supply. Data from the U.S. Department of Labor shows that in 2019, New Mexico had among the fewest mental health and substance abuse social workers of any state. Its mental health care professionals only meet 12% of the state’s need, according to the Kaiser Family Foundation.
Erika Wilson said that staffing emergency response is even more difficult because many of the critical shifts are off-hours. “It’s not like a mental health crisis happens at 1 p.m. on Tuesdays; they happen 24/7.” And Ley, of New Mexico Solutions, said he would have concerns about deploying crisis responders to 911 calls before police determined they were safe. “If something bad happens to my staff or to a patient in one of those situations, the potential legal liability could end my entire company.”
That is what makes it appealing to pair law enforcement and clinicians, as in the Mobile Crisis Teams that Bernalillo County and the city of Albuquerque both support. In their first two years, the teams responded to over 5,000 calls for service, according to a preliminary evaluation by UNM’s Institute for Social Research. But they were limited by personnel, according to Lt. Dietzel. “Having enough clinicians to keep Mobile Crisis Teams running at current capacity has been a battle,” he said, pointing out that APD had funding for four teams but only has staff for two.
That has proven far too few to meet the community’s needs. A team wasn’t dispatched to Elisha Lucero the night she died because none were working: their shift ended before her family called for help at 1 a.m. Bernalillo County’s director of behavioral health services, Margarita Chavez, who was herself an EMT and medic for many years, estimates the city and county need to triple the number of teams in order to provide service 24/7. She’d like to see that program expanded as part of the new department. “It’s my hope that the city does incorporate a lot of what we’re doing, as opposed to reinventing the wheel.”
Albuquerque has to recognize the limits of what even ambitious changes in policing will accomplish, said Tim Black, the director of consulting of CAHOOTS. “Crisis emerges when a need goes unmet,” he said, and that can only be resolved by more comprehensive behavioral health services and a stronger social safety net. “If there aren’t any other resources beyond the jail and hospital, it will still be cycling people back through those same broken systems.”
But failing to act would be unacceptable. The family of Elaine Maestas ultimately won a $4 million settlement for the death of her sister, Elisha, but the Bernalillo County Sheriff’s Office adamantly refused to admit any fault. Now more than a year later, Maestas finds some solace in devoting herself to change, but the pain of the loss will never leave her. “I have still just barely started to find myself.”
***
This reporting was supported by the Jacob and Valeria Langeloth Foundation.
