Christina spent much of 2023 traveling to Santa Fe for medical care during her pregnancy. She’d leave home about two hours before each doctor’s visit for the roughly 100-mile one way trip from her home in northern New Mexico’s rural Mora county, in case accidents or construction caused traffic slowdowns.
Two years ago, she would have received her care 30 miles down the road at Alta Vista Hospital in Las Vegas. But the hospital closed its delivery care unit in June 2022.
“People say it’s because they weren’t getting paid enough, I don’t really know why but they closed,” said Christina, who asked New Mexico In Depth not to use her last name to protect her and her newborn’s privacy. “So I have to go to Santa Fe.”
Her high-risk pregnancy forced the trip to Santa Fe three times a week in her final months, with transportation costs running about $150 a week.
The transportation was unhealthy too. “They tell you they don’t want you to sit that long, but what do you think I’m doing? Sitting,” she said.
Once at Santa Fe Medical Center, Christina sometimes waited up to 30 minutes to see a specialist.
Now, with the birth of a healthy baby in November, the cycle has started over – long drives to Santa Fe for infant and mother checkups for another year.
Christina isn’t alone. Across the state, one in three New Mexico counties are “maternity care deserts,” according to a 2022 March of Dimes report on maternal care nationwide. Nearly 18% of women in New Mexico lack access to birthing hospitals within 30 minutes of where they live, compared to the national 9.7%, according to the report.
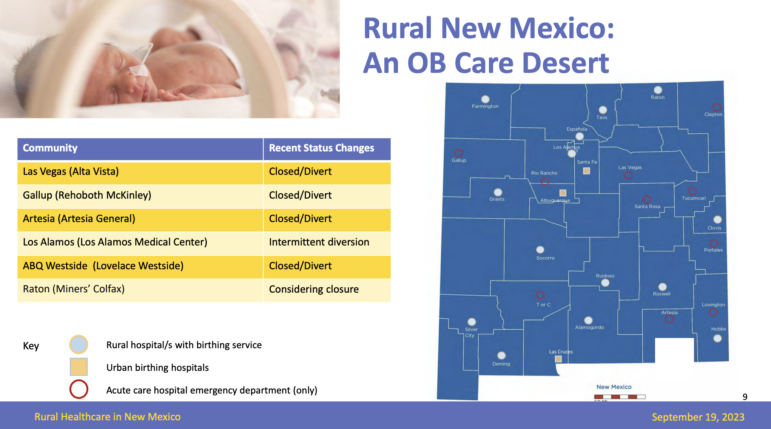
In addition to Alta Vista, hospitals in Gallup and Artesia recently closed their birthing units, leaving 14 rural birthing hospitals across the state. Raton’s hospital is currently considering closing its delivery unit, according to a presentation by the New Mexico Hospital Association to the Legislative Health and Human Services Committee in September.
High costs not fully covered by Medicaid or other revenue sources are the chief challenge to sustaining rural hospitals and the specialized care needed for delivering babies, hospital administrators told lawmakers at the September hearing.
Public officials agree. “We’ve had several hospitals close their obstetrics wings, as a result of needing to make some changes for their own operating costs,” said Lorelei Kellogg, acting Medicaid Director at the New Mexico Human Services Department.
When hospitals close their delivery units, there are cascading effects. Not only must women travel long distances to deliver their babies at a hospital, but access to care over the nine months of pregnancy declines as well. That’s because Medicaid, the government run low-income health insurance program, pays much less for pre-delivery care than the actual birth of a baby. More than 40% of New Mexico’s population uses Medicaid.
When rural providers can’t count on income from the delivery of a baby at a nearby hospital, it becomes difficult for them to offer important prenatal care over the prior nine months.
A dwindling rural population lies at the root of hospital struggles to maintain birthing facilities.
According to New Mexico State University, 20 counties experienced significant population decline from 2010 to 2018, a trend that continues today. Rural counties have aging populations and fewer births, making it difficult for hospitals to sustain specialized maternity care units.
In 2020, nine hospitals in rural New Mexico reported delivering fewer than 300 babies, said Troy Clark, the executive director at the New Mexico Hospital Association, which is considered low. But to keep their birthing units open, hospitals need to maintain certain staff on hand regardless of how many babies they deliver.
“You don’t just need an obstetrics gynecologist to run a birthing center, you need anesthesiologists, nurse practitioners and family physicians to be available around the clock. And that cost adds up,” Clark said.
In short, it’s expensive to maintain a hospital birthing unit. When hospitals face hard choices to keep their doors open, they are more prone to shut down the more expensive services to maintain others.
Compounding growing financial stress, in 2020, rural hospitals began receiving less money from the Centers for Medicare and Medicaid Services (CMS), the federal agency in charge of the government’s health insurance programs for seniors and low-income people.
The agency instead began sending more money to high-volume hospitals as a response to the COVID-19 crisis. Generally, hospitals rely on these payments to sustain their operations, as payment for providing Medicaid services in New Mexico isn’t enough to keep a hospital running. The change placed a financial strain on rural hospitals, which typically serve fewer patients than urban hospitals.
“Rural hospitals depended on a fixed payments system to survive. They are now in crisis,” said Christina Campos, the administrator at Guadalupe County Hospital.
In 2023, state lawmakers increased the rate paid to providers for Medicaid services, but the amounts still aren’t enough to cover hospital costs.
Finding money for rural hospitals
To shore up facilities still operating birthing units, the hospital association and the New Mexico Human Services Department want to leverage a federal matching program that gives hospitals $4 for every $1 raised by the state.
“We are roughly looking to raise somewhere between $300 million to $500 million in state funds for matching,” said Clark. Kellogg said the funding scheme would require them to keep their birthing units open. “That’s really the intention behind those supplemental payments,” she said, adding “The requirement, or the metric that’s tied to the supplemental OB payment is really that they cannot minimize their services.”
Healthcare administrators say it’s also important to increase Medicaid rates for prenatal care.
Right now, Medicaid pays for prenatal and delivery care together in one package. Clinics and hospitals that provide both services to the same patient receive full payment from Medicaid. Clinics that provide prenatal services sometimes shut down soon after delivery units close when they can no longer deliver babies at a nearby hospital.
That was the case for Alumbra Women’s Health and Maternity Care center, a midwifery clinic based in Las Vegas, which shut down 15 months after Alta Vista Hospital first suspended their delivery care unit in 2016.
Connie Trujilio, the clinic’s founder and a certified nurse midwife from Las Vegas, used to provide prenatal services at her clinic, and delivered babies at Alta Vista hospital.
When the delivery unit at Alta Vista hospital unexpectedly shut down in 2016 because of lack of staff and a low demand for services, her patients had to travel to Santa Fe to deliver without Trujillo, who couldn’t sustain her practice from the low Medicaid payments for prenatal care. Alta Vista hospital eventually reopened their delivery unit again in 2017 for a few years before permanently closing again in 2022. But by 2018, Trujillo’s practice was already closed.
“We took care of so many people in Las Vegas and it was just such a huge loss. I sometimes think of patients I’ve had for years and wonder, where are they getting care?” said Trujilio.

One solution may be using phones or the internet to offer prenatal care at home, called telehealth.
The Rural Ob Access & Maternal Service, or ROAMS for short, is a collaborative project of hospitals and clinics in northeast New Mexico meant to increase access to prenatal care. It created a telehealth program in 2019 that uses computers or phones to connect health clinics and hospitals in Clayton, Raton, and Taos with women at home. It also deploys community healthcare workers who help pregnant people navigate various tasks like accessing transportation for appointments, or ensuring they get the right nutrition. This is particularly important in rural New Mexico where communities grapple with higher poverty rates.
According to Colleen Durocher, the executive director of ROAMS, the program significantly increased the number of women receiving prenatal care through the Raton hospital, through a combination of telehealth visits during the pandemic, public education, and services from community health workers.
Now, with a federal grant that supported ROAMS just ended, ROAMS is looking for how to keep its momentum going. Because Medicaid payments for pregnancy and delivery are bundled together, health clinics that only provide prenatal care struggle to sustain their services.
“We need to look at untangling the global rate of reimbursements so that prenatal services are reimbursed properly,” said Durocher
ROAMS is currently exploring how to offer telehealth to women with high risk pregnancies. According to various studies, women in rural communities are prone to increased rates of high risk pregnancies, which require visits to specialized doctors who in New Mexico are largely in urban areas.
“We see high risk patients who need to be seen by a maternal fetal specialist. However, these specialists are only in urban areas like Albuquerque,” said Jay Fluhman, a certified nurse practitioner with ROAMS.
Telehealth is capable of serving those with high risk pregnancies, but it requires specialized equipment that rural communities usually don’t have. As a result, women with higher risk pregnancies, like Christina in Mora county, have to travel long distances for care.
Christina said that had Alta Vista offered simply an ultrasound service it would have been a big help.
“If that was closer, that would save you one trip right there,” she said. “One trip makes a difference, it costs money to go over there all the time.”
Marjorie Childress contributed to this report.
This article was updated to correct Connie Trujillo’s first name, and to correct that the federal match for hospitals is $4, rather than $7, for every $1 spent by the state.